Fund a Heart for Tommy
Fundraising campaign by
MelissaJArias
-
US$11,781raised of $65,000.00 goal goal
Campaign Story
Fund-A-Heart
For Tommy Stemmle
The average heart transplant costs $874,800 for the first year.
With insurance, out of pocket costs will be around $65,000.
Tommy's Story:
On April 15th, 2011, Tommy left Las Vegas and traveled to Michigan to work as an engineer on the Great Lakes. Two weeks later, my phone rang at 6:30 am. Tommy had been experiencing chest pressure throughout the night and was now being airlifted to the University of Michigan Cardiovascular Center. Our family was stunned. The words stung, “critical”, “echocardiogram”, and “cardiovascular functioning”. We were all obviously confused and in a panic.
Unlike the Grinch who stole Christmas, having a heart grow 2 sizes larger (aka cardiomyopathy) can be fatal. His heart was functioning below 8% of its capacity. All caused by a virus! After a week of observation at U of M, he became stable enough to travel back to Las Vegas to continue his critical care. Even with treatment, his heart function only increased to 20%; he received an implantable defibrillator in August. He attended cardiac rehab 3 times a week.
Tommy went from 200 lbs. to losing over 30lbs. His eating habits, of course, had to change. He went from being able to eat anything he wanted to a diet containing no sodium and no more than 2 liters of any fluid a day.
Tommy’s health insurance covered 80% of all medical bills-which sounds great until you realize that one month’s bills can total $35,000.
Fast foward to November 2012, Tommy went back into the hospital after not being able to keep any food down for 5 days straight, his heart has relapsed back into heart failure and is now functioning under 15%. His doctor wants Tommy to get evaluated for a heart transplant, except, heart is the only transplant his insurance company does not cover. He now sleeps with oxygen and needs a wheelchair when he needs to get around. He will be retuning to NY to go under Medicaid/Medicare.
Medical Updates:
Updated 11/19/12
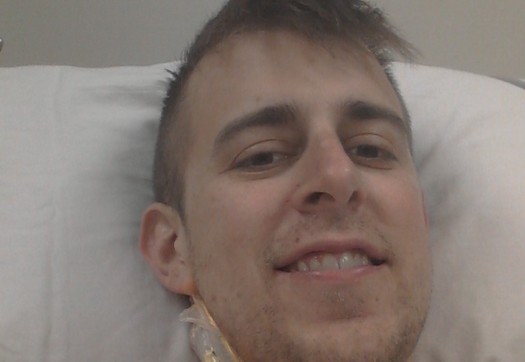
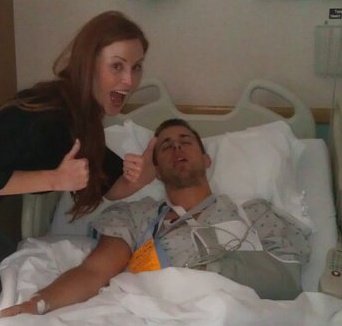
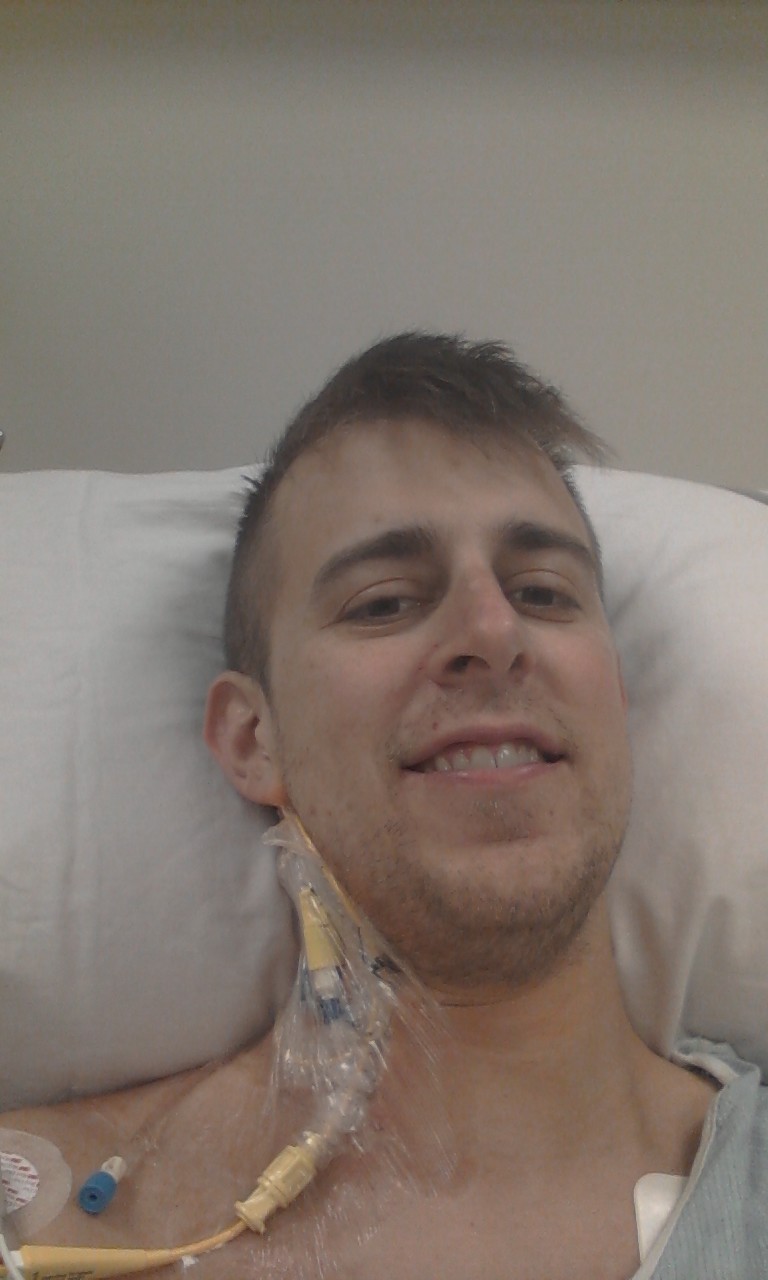
Tommy recently had his heart pressure measured (a very painful test going through the neck to the heart, photo above). The results were much lower than anticipated and he is being transfered to Columbia University Medical Center in Manhattan.
Update from Tommy 12/20/12
So I have arrived at Columbia University, I’m finally where I need to be to get proper treatments. I am currently in advanced heart failure, with a life expectancy of less than a year if nothing is done to correct it. Being blood type O+, and being ginormous, are basically the 2 worst things you can have when needing a heart transplant. They expect I would be waiting on the transplant list for 2+ years. I am currently on 2 strong heart medications via an IV drip through my neck with tubes directly into my heart to deliver the medicine. This treatment has made me feel sooooo much better since being on it, I almost feel like my old self again. I can finally walk without being out of breath, I have my appetite back, and I can spend a full day without being nauseous. ...
Update 1/2/12
Tommy's LVAD surgery went well and he will be in the ICU for the next week before being transfered to general recovery. He is sitting on his own. What is LVAD Surgery? The left ventricle is the large, muscular chamber of the heart that pumps blood out to the body. A left ventricular assist device (LVAD) is a battery-operated, mechanical pump-type device that's surgically implanted. It helps maintain the pumping ability of a heart that can't effectively work on its own.
During the procedure
The procedure to implant a VAD is an open-heart surgery that took about six hours. He was connected to a machine that helps him breathe (ventilator) during surgery. A tube will be run down the throat to the lungs and connected to the ventilator. He had the ventilator removed the following day. A cut will be made down the center of his chest. His chest bone (sternum) is separated and his rib cage is opened so that your doctors can operate on his heart. His heart was stopped during the surgery. He was connected to a heart-lung bypass machine that keeps oxygenated blood flowing through your body during surgery.
Once your VAD is implanted and working properly, the doctors will take you him the heart-lung bypass machine so that the VAD can begin pumping blood through your heart.
Some VADs pump blood similar to the way your heart does, with a pumping action. Other VADs allow a continuous stream of blood to flow through your heart. If you have a continuous stream of blood flowing through your LVAD, you may not have a normal pulse, even though your body is getting the blood it needs.
After the procedure
When you wake up from your surgery, you'll be in the intensive care unit (ICU). You'll stay in the ICU for several days, where you'll be fed and given fluids and medications through an intravenous (IV) line. You'll have a tube in your bladder to drain your urine and other tubes in your chest to drain fluid and blood. Your lungs may not work properly immediately after your surgery, so you may need to remain connected to a ventilator for a few more days until you're able to breathe on your own.
After a few days in the ICU, you'll likely be moved to a regular hospital room. As you recover, nurses will help you become increasingly active. They may help you get out of bed, sit up and walk around the hallways of the hospital. You may also have visits with a physical therapist to help you continue to gain strength and get used to performing daily activities. The amount of time you'll spend in the ICU and in the hospital can vary, depending on your condition before the procedure and how well you recover after your VAD is placed.
You'll likely be prescribed antibiotics and blood-thinning medications to prevent infection and other complications while you're in the hospital. Your doctor will order blood tests periodically to check your kidney function and to make sure your medications are effective
Trouble with donating online??
Donations can be sent directly to Tommy's sister through PayPal at [email protected] and will be added to Tommy's medical account.
Organizer
- MelissaJArias
Donors
- Carroll Family
- Donated on Jun 15, 2013
- Gina and Alexandria Bartkus
- Donated on Apr 26, 2013
Tommy Sr. is an amazing man and so this story is literally heartbreaking. Tommy Sr. runs the PAL out of a sincere love for helping children. He sponsors my daughter, who has special needs, in karate. This gift has helped improve her core muscle strength and coordination tremendously. He is always the first one to reach in to his pocket for any cause, especially ones that benefit children! PLEASE ENCOURAGE THE SHARING OF THIS LINK, AND HELP A MAN WHO DOES SO MUCH FOR OUR CHILDREN, SAVE HIS CHILD. A virus may have damaged Tommy's heart, but sending this link viral can replace it :)
3 months out
Update posted by MelissaJArias at 08:24 pmWell, it has been a few months since my last update to this website. I primarily use my Facebook to keep everyone updated of day to day activities. Recovery definitely started out slow for me, and took about 2 months for me to finally start feeling better. My doctors and. . . . .
Hospital Journal - Part 3
Update posted by MelissaJArias at 06:58 pm1/11/13- At 7AM, mom and OK Lori left to go home. I was incubated and out cold. Around 2PM, I had Chris from the nurses’ station call mom to see if she was still in the hospital or at home. Mom said she was home and would be back to. . . . .
The Plot Thickens...
Update posted by MelissaJArias at 05:01 pm1/10/13- Discharge Day! Dr. Jorde came in this morning and seemed to have given me credit for fixing the swelling in my legs, since I was the one telling him for days to diurese me. Whatever, the swelling is gone and I am going home soon, so I am happy.. . . . .
Hospital Journal - Part 2
Update posted by MelissaJArias at 05:27 pm1/1/13-New Years Day After some Adderall and Ativan, I got in about two and a half hours of sleep, which I was satisfied with. I have been trying to do as much as I can on my own. As of noon I had performed my respiratory and physical therapy exercises. . . . .
Hospital Journal
Update posted by MelissaJArias at 06:26 pmI was hoping to keep the site updated daily with journal entries. Obviously, I have had some hard and trying days, making that near impossible to do. I did however, keep a journal daily to the best of my ability to track my own progress, as well as share with. . . . .
12/25/12
Update posted by MelissaJArias at 04:51 amSo I have arrived at Columbia University, I’m finally where I need to be to get proper treatments. I am currently in advanced heart failure, with a life expectancy of less than a year if nothing is done to correct it. Being blood type O+, and being ginormous, are basically. . . . .
Donors & Comments
- Brian R
- Donated on Nov 28, 2019
Stay strong shipmate!
- Carroll Family
- Donated on Jun 15, 2013
- Gina and Alexandria Bartkus
- Donated on Apr 26, 2013
Tommy Sr. is an amazing man and so this story is literally heartbreaking. Tommy Sr. runs the PAL out of a sincere love for helping children. He sponsors my daughter, who has special needs, in karate. This gift has helped improve her core muscle strength and coordination tremendously. He is always the first one to reach in to his pocket for any cause, especially ones that benefit children! PLEASE ENCOURAGE THE SHARING OF THIS LINK, AND HELP A MAN WHO DOES SO MUCH FOR OUR CHILDREN, SAVE HIS CHILD. A virus may have damaged Tommy's heart, but sending this link viral can replace it :)
- Keith S
- Donated on Apr 25, 2013
- Shannon Daly
- Donated on Mar 17, 2013
If you have the money to buy boots or clothes; you have the money donate. Help save a life!
- Chris Pierce
- Donated on Feb 23, 2013
Keep up the fight man!
- Devereaux Family
- Donated on Feb 20, 2013
Sending our love and prayers to you all! xoxoxo
- Boris Sabovic
- Donated on Feb 11, 2013
- Sweetpeashope
- Donated on Feb 07, 2013
Hope you can get all the help you need. As me and my organization ( Sweetpeashope ) we are doing what we can on our side, posting on our walls and talking to friends to help out. May God will be with you all the step of the way. Sending prayers ad love.
- Guest
- Donated on Feb 05, 2013





Stay strong shipmate!