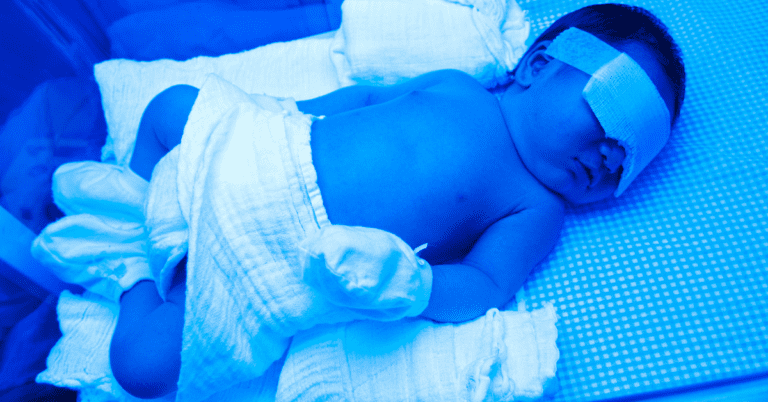
Beth’s Story
Fundraising campaign by
Jennifer Chynoweth
-
US$0.00raised of $20,000.00 goal goal
Campaign Story
When Beth Jones* gave birth to her first child in 2013, she and her
husband felt blessed with a miracle. Beth had two miscarriages before
delivering Emma, who was born at term weighing nearly 10 pounds. Their
newborn seemed healthy in every regard.
What a difference a few days made. By the time Emma was 5 days old, her skin had turned orange, and her parents began to suspect that this was no routine case of infant jaundice — a condition that often disappears quickly as the newborn’s liver matures.
It took six months — and many hospital visits, inconclusive tests and finally a visit to a special clinic in Pennsylvania Dutch Country — before the Joneses learned that Emma had Crigler-Najjar syndrome – Type 1 (CN), a rare, life-threatening genetic condition that affects the liver.
CN is characterized by high levels of bilirubin in the blood and can lead to brain damage (known as kernicterus), hearing loss, developmental problems and other issues. It’s mostly managed with the same kind of light therapy (or phototherapy) that’s often used to treat infant jaundice. But the only existing cure for CN is a liver transplant, which Emma successfully received when she was just 3 years old.
While the transplant enables Emma to function without the use of phototherapy and without the fear of death from toxic unconjugated bilirubin levels, she still has the gene mutation that caused her CN and could pass the abnormality on to her children.
Nothing was Easy
Even before the diagnosis, Emma’s doctors insisted that she be treated with phototherapy lights. Yet, the hospital wouldn’t issue the family a set of lights for home use, citing liability concerns. The family checked with medical-device companies, but again came up empty-handed.
That meant the Joneses had to return to the hospital nearly every two weeks so that Emma could sleep under phototherapy lights. Beth often spent two weeks at a time in the hospital with Emma — where the difficulty of getting a baby to sleep under bright lights was compounded by frequent interruptions from doctors, medical residents and others. Beth calls this episode one of the most frustrating aspects of her daughter’s medical journey.
“I was so depressed,” she recalls. “I didn’t want to get up [in the morning]. I couldn’t take care of [Emma]. My hair was falling out. It was terrible because nobody could tell me what was wrong with my baby.”
Doctors ran a battery of tests, at one point even testing Emma for Syphilis, a sexually transmitted disease. “I thought it was absolutely ridiculous, but that just tells you we were out of options,” said Beth.
HELP AND HOPE IN AN UNEXPECTED PLACE
When Emma was 6 months old, her mother — with the help of a patient advocate at the hospital that initially treated Emma — found the Clinic for Special Children in Lancaster County, PA.
A medical home for children with rare genetic diseases, the nonprofit clinic began as a partnership between Dr. Holmes Morton (a Harvard-trained pediatrician), his wife Caroline and the Amish and Mennonite communities they served. Although CN affects an estimated one in a million children, the rare genetic disorder is more prevalent in the tight-knit Mennonite and Amish communities.
At the Clinic for Special Children, Emma finally received a diagnosis of CN and was treated by a doctor who helped her parents manage the condition through a routine of light exposure (phototherapy and natural light) and bloodwork and some dietary changes.
Emma’s doctor at the clinic also gave the Joneses hope that their daughter would pull through. According to Beth, he said that Emma would likely need a liver transplant at some point, but that the survival rate for CN liver-transplant patients was very high, thanks in part to advances in immunosuppressant drugs.
“He told me she was going to make it,” recalls Beth, her voice cracking. “The others didn’t know what was wrong with her. At one point, I was told she was going to live for three months unless we did a transplant immediately.”
Donate And Help Beth's
Organizer
- Jennifer Chynoweth
- Campaign Owner
No updates for this campaign just yet